Week4
Back to NS210b Class page
MANUSCRIPT ID
- Title
- Reference
- Abstract
- Keywords
- Input Author
MANUSCRIPT DETAILS
- Introduction/Aims
- Methods
- Results
- Summary
- Discussion
MANUSCRIPT ID
- Title
Association of plasma leptin levels with incident Alzheimer disease and MRI measures of brain aging.
- Reference
JAMA. 2009 Dec 16;302(23):2565-72.
- Abstract
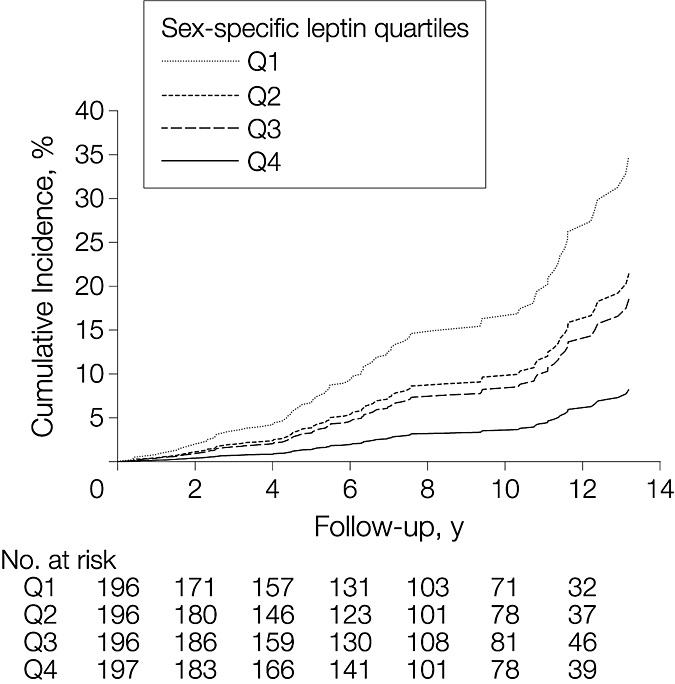
CONTEXT: The adipokine leptin facilitates long-term potentiation and synaptic plasticity in the hippocampus, promotes beta-amyloid clearance, and improves memory function in animal models of aging and Alzheimer disease (AD). OBJECTIVE: To relate baseline circulating leptin concentrations in a community-based sample of individuals without dementia to incident dementia and AD during follow-up and magnetic resonance imaging (MRI) measures of brain aging in survivors. DESIGN, SETTING, AND PARTICIPANTS: Prospective study of plasma leptin concentrations measured in 785 persons without dementia (mean [SD] age, 79 [5] years; 62% female), who were in the Framingham original cohort at the 22nd examination cycle (1990-1994). A subsample of 198 dementia-free survivors underwent volumetric brain MRI between 1999 and 2005, approximately 7.7 years after leptin was assayed. Two measures of brain aging, total cerebral brain volume and temporal horn volume (which is inversely related to hippocampal volume) were assessed. MAIN OUTCOME MEASURE: Incidence of dementia and AD during follow-up until December 31, 2007. RESULTS: During a median follow-up of 8.3 years (range, 0-15.5 years), 111 participants developed incident dementia; 89 had AD. Higher leptin levels were associated with a lower risk of incident dementia and AD in multivariable models (hazard ratio per 1-SD increment in log leptin was 0.68 [95% confidence interval, 0.54-0.87] for all-cause dementia and 0.60 [95% confidence interval, 0.46-0.79] for AD). This corresponds to an absolute AD risk over a 12-year follow-up of 25% for persons in the lowest quartile (first quartile) vs 6% for persons in the fourth quartile of sex-specific leptin levels. In addition, a 1-SD elevation in plasma leptin level was associated with higher total cerebral brain volume and lower temporal horn volume, although the association of leptin level with temporal horn volume did not reach statistical significance. CONCLUSION: Circulating leptin was associated with a reduced incidence of dementia and AD and with cerebral brain volume in asymptomatic older adults.
- Keywords
Alzheimer's disease, leptin, metabolism, aging, brain volume
- Input Author
KCO
MANUSCRIPT DETAILS
- Introduction/Aims
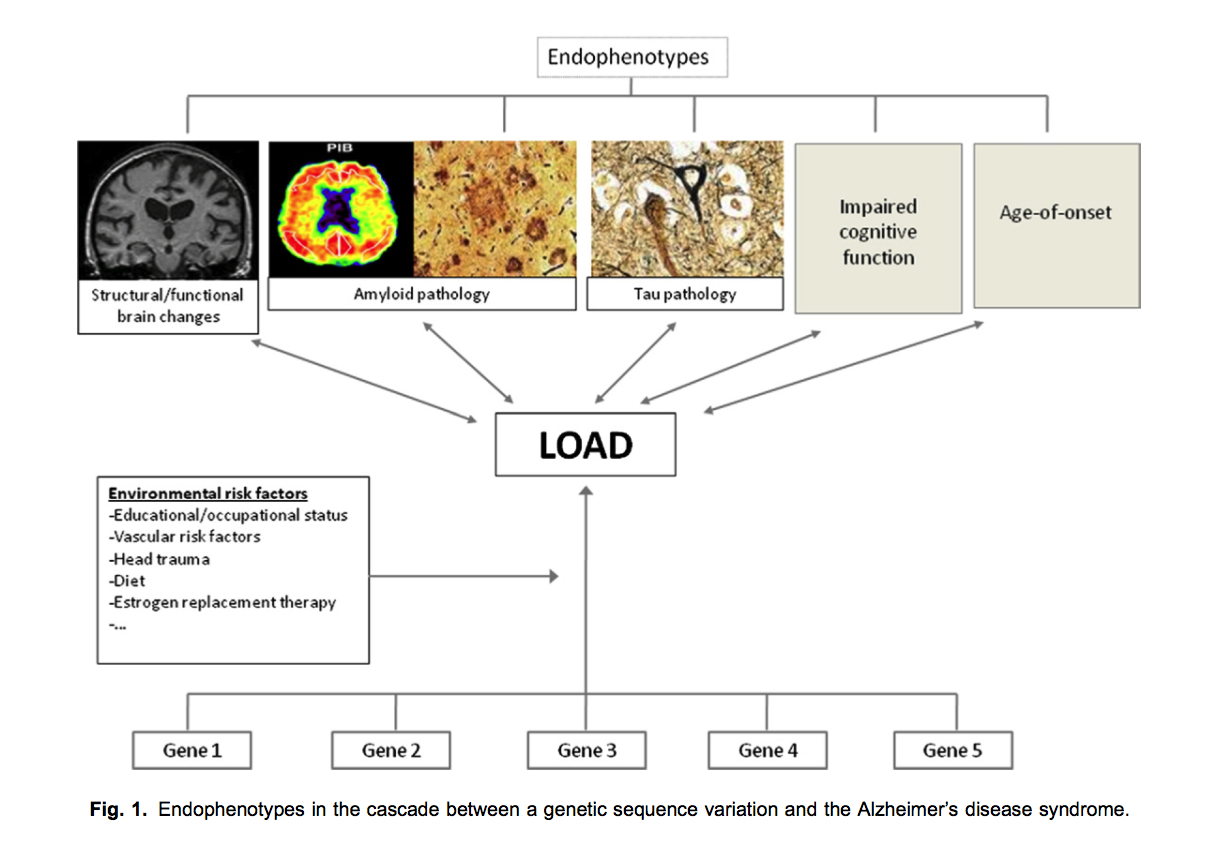
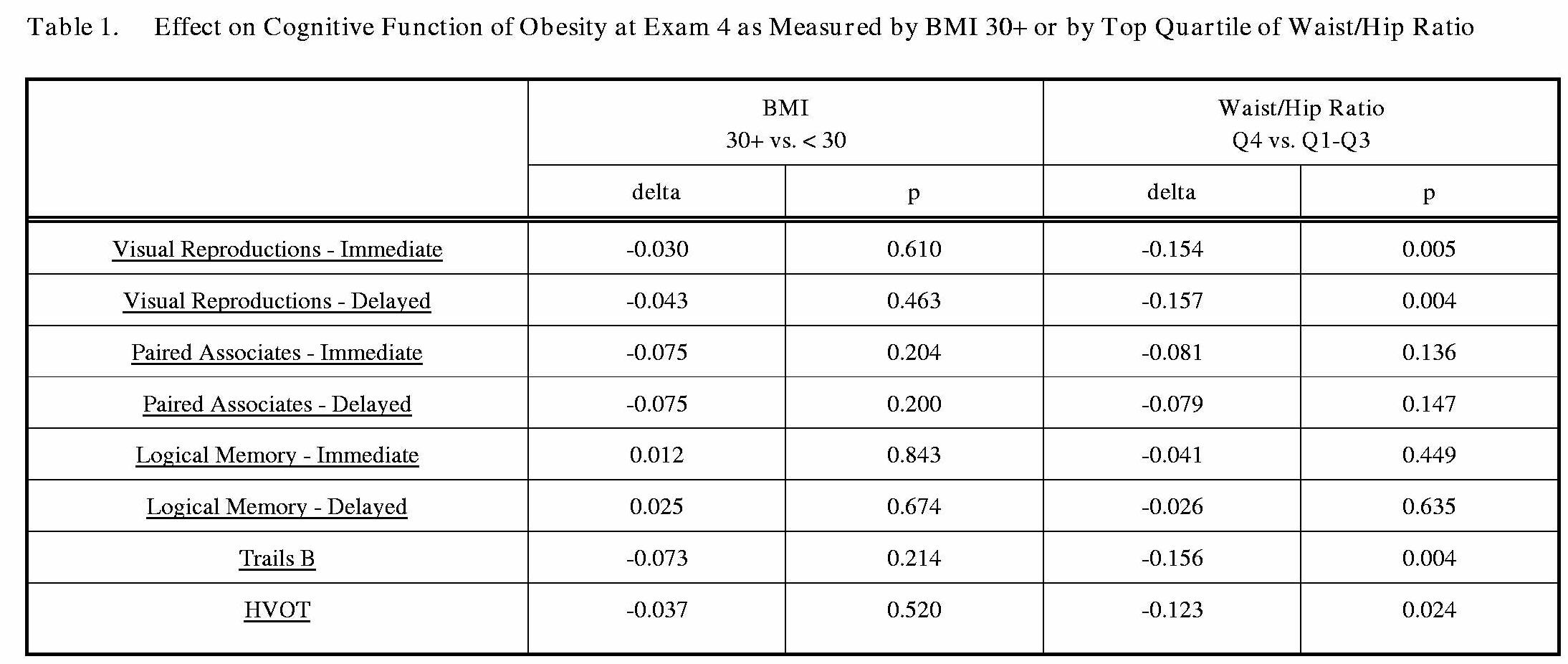
Obesity and insulin resistance have been identified as risk factors for Alzheimer's disease, and prospective studies have shown that mid-life obesity is associated with increased risk of dementia and poorer cognitive function in the general population (see Figure 1, from Wolf et al., 2007 [1]).
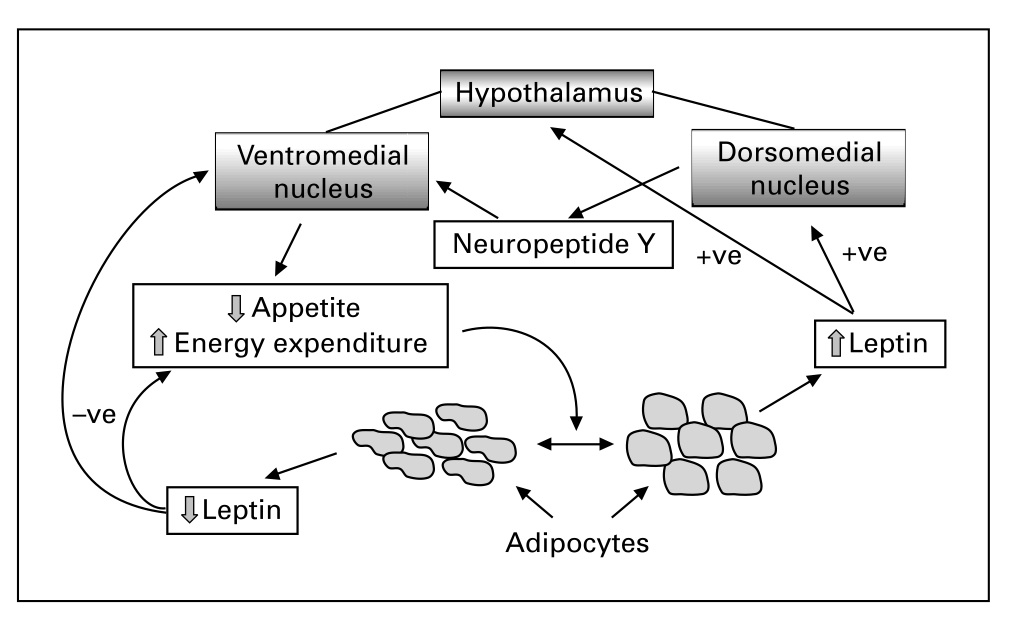
Leptin is an adipokine with a role in the regulation of signaling caloric intake and fat stores to the hypothalamus. This signaling alters food consumption, with high levels of leptin indicating satiety (see Figure 2, from Power et al., 2001)[2].
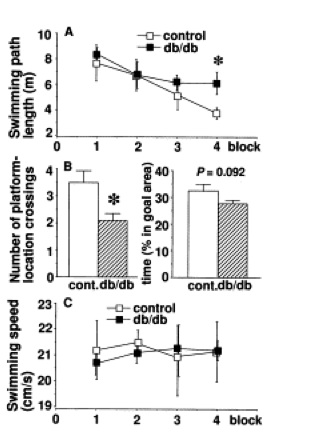
More recently, a role of leptin in memory facilitation has been identified. In addition to its role in the hypothalamus, leptin has been shown to act in the CA1 region of the hippocampus, and mice with defective leptin receptors show diminished long-term potentiation and poorer performance on memory tasks (see Figure 3, from Li et al., 2002)[3].
Changes in brain morphology have been suggested as putative endophenotypes of Alzheimer's disease (see Figure 4, from Reitz et al., 2009)[4]. This study uses data from participants who underwent structural MRI to investigate the relationship between brain volume and dementia.
In this study, researchers aimed to relate baseline plasma leptin levels in individuals free of dementia to the later incidence of dementia and Alzheimer's disease, and to relate those results to the morphological appearance of the brain.
- Methods
Participants were part of the Framingham Heart Study [5] [6] initiated in 1948. Leptin levels were measured in 785 participants without dementia in the twenty-second examination cycle (1990-1994).
Of those individuals, 198 underwent volumetric MRI between 1999 and 2005. For the purposes of this study, the morphometric characteristics evaluated were total cerebral brain volume and temporal horn volume.
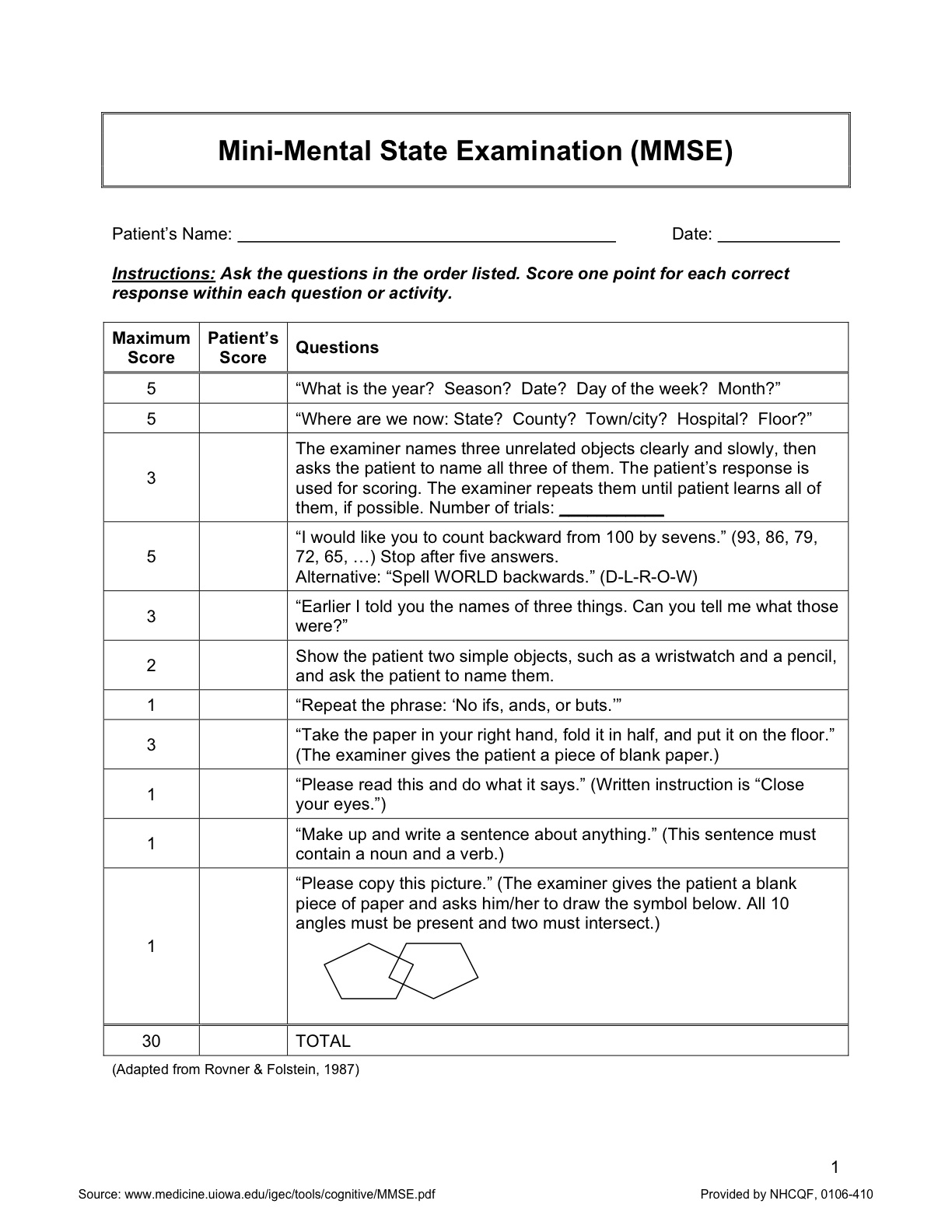
Participants were screened for cognitive decline with standardized neuropsychological testing, and evaluated biennially thereafter with the Folstein Mini Mental State Exam (see Figure 5). If this test, the participant, physician, or family raised the possibility of cognitive decline, more thorough neurological and neuropsychological testing was performed. Data acquired through December of 2007 were used for this study.
- Results
Incidence of dementia and AD were inversely related to log leptin, after leptin levels were standardized for sex (see Figure 6). There was no effect modification by the APOE4 allele.
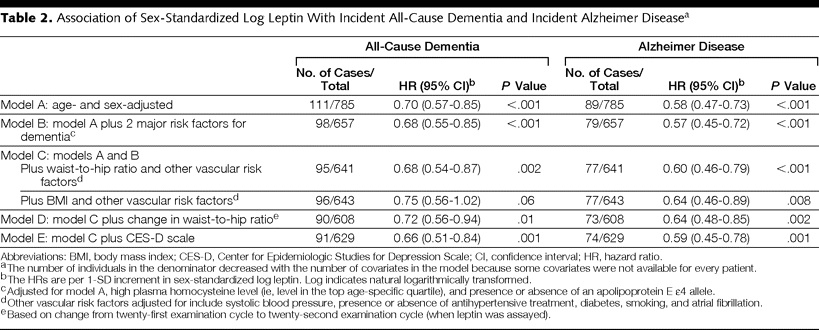
Four models were used to control for different variables in evaluating the relation of leptin to risk of AD or dementia (see Table 2):
Model A: Age and sex
Model B: Age + sex + homocysteine level + APOE e4 carrier status
Model C: Model B + waist-to-hip ratio or BMI + systolic blood pressure + other vascular risk factors
Model D: Model C + change in waist-to-hip ratio from 21st to 22nd examination cycles
Model E: Model D + baseline depression status
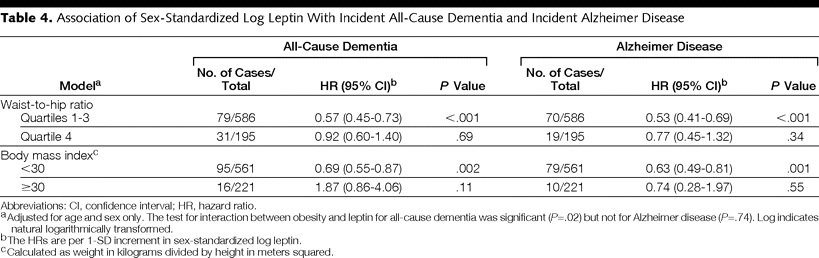
After stratifying the groups according to waist-to-hip ratio (see Table 4), a strong inverse association between leptin and these groups was observed in the lower three quartiles.
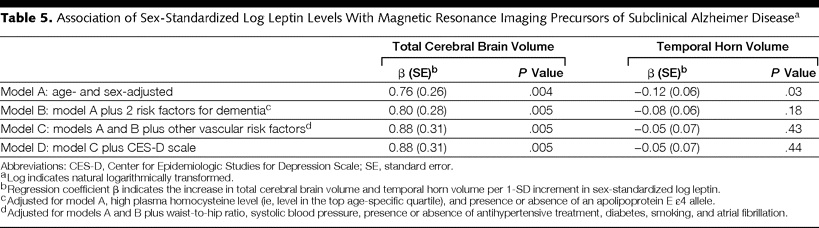
Leptin levels were positively associated with total cerebral brain volume in all models, and inversely associated with temporal horn volume in the age- and sex-adjusted models. Inverse association with THV was not significant after adjusting for neurodegenerative or vascular risk factors (see Table 5).
- Summary
Higher baseline leptin levels were prospectively associated with a lower incidence of AD and dementia, even after adjusting for vascular risk factors and for waist-to-hip ratio.
The association was not statistically significant in participants with the highest waist-to-hip ratios and BMI >30; however, there were relatively few events in those groups.
Higher leptin levels were also associated with larger brain parenchymal volume, and smaller ventricular volume.
- Discussion
In thin people in this elderly population of European descent, high leptin is protective; low leptin is a risk factor.
The relationship does not hold in obese people, who may be expected to have high leptin, but who are resistant to its anorexic effects—and therefore may be resistant to its neuroprotective effects as well.
Because PET imaging or quantification of A-beta or tau in the CSF would be difficult to adapt for screening millions of patients, the search for peripheral biomarkers of AD and dementia is critical. Current searches for such biomarkers have not yet produced any validated tests, and it is unlikely that a single biomarker will ever suffice. Plasma leptin is a possible candidate biomarker, but must be validated before it can be clinically useful.
The apparently robust inverse relationship between plasma leptin and AD risk may also provide insight into the mechanisms of neurodegeneration seen in AD and other forms of dementia. It remains to be seen whether leptin directly mediates the neuroprotective effects seen here, or whether it is a marker of another protective process.
The study is limited by the fact that leptin levels were only measured once, brain MRI's were available for a single time point, and the population lacks the ethnic diversity that would allow these results to be extended more broadly. The findings need to be independently confirmed, but may ultimately provide another biomarker of healthy brain aging.
- References
Akomolafe A, Beiser A, Meigs JB, Au R, Green RC, Farrer LA, Wolf PA, Seshadri S. Diabetes mellitus and risk of developing Alzheimer disease: results from the Framingham Study. Arch Neurol. 2006 Nov;63(11):1551-5.
Jagust WJ, Landau SM, Shaw LM, Trojanowski JQ, Koeppe RA, Reiman EM, Foster NL, Petersen RC, Weiner MW, Price JC, Mathis CA; Alzheimer's Disease Neuroimaging Initiative. Relationships between biomarkers in aging and dementia. Neurology. 2009 Oct 13;73(15):1193-9.
Li XL, Aou S, Oomura Y, Hori N, Fukunaga K, Hori T. Impairment of long-term potentiation and spatial memory in leptin receptor-deficient rodents. Neuroscience. 2002;113(3):607-15.
Power DA, Noel J, Collins R, O'Neill D. Circulating leptin levels and weight loss in Alzheimer's disease patients. Dement Geriatr Cogn Disord. 2001 Mar-Apr;12(2):167-70.
Reitz C, Mayeux R. Endophenotypes in normal brain morphology and Alzheimer's disease: a review. Neuroscience. 2009 Nov 24;164(1):174-90.
Wolf PA, Beiser A, Elias MF, Au R, Vasan RS, Seshadri S. Relation of obesity to cognitive function: importance of central obesity and synergistic influence of concomitant hypertension. The Framingham Heart Study. Curr Alzheimer Res. 2007 Apr;4(2):111-6.